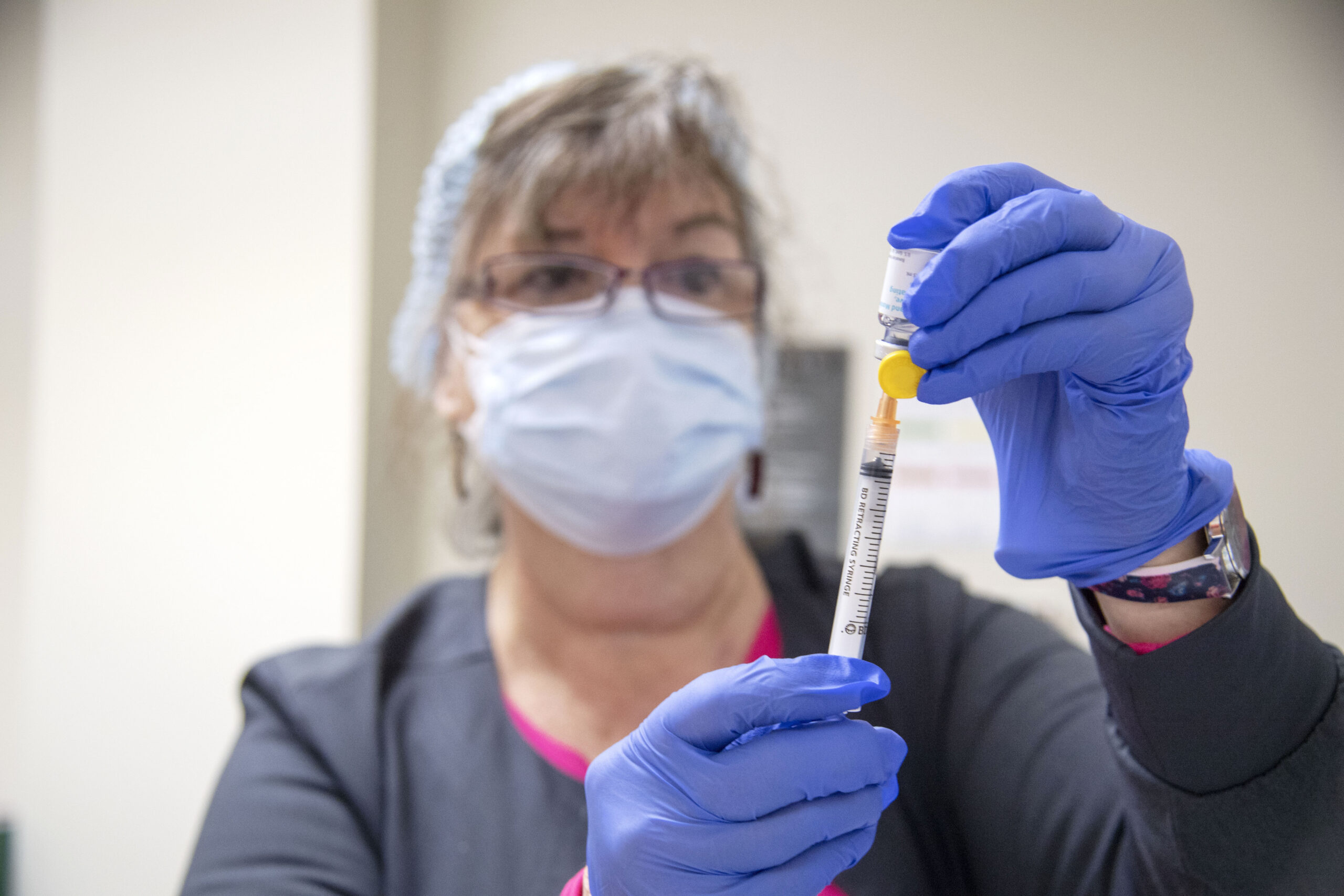
A document circulating on social media and elsewhere is being cited as a smoking gun to suggest Pfizer knew its COVID-19 vaccine causes more “adverse events” than previously stated, a claim some experts say requires a more nuanced look.
Released by the U.S. Food and Drug Administration as part of a recent U.S. court order, the one-year-old, 38-page report of post-marketing data from Pfizer includes an appendix listing hundreds of reported adverse events from its COVID-19 vaccine, all of which are defined as being of “special interest.”
Whether the data is being, or can be, accurately interpreted is a point some experts are flagging as an issue with the document, particularly given the amount of real-world data gathered since then.
Experts say not every adverse event cited in the report can be chalked up to the vaccine, while others are consistent with the vaccine’s known side-effects.
CTVNews.ca spoke to two infectious disease specialists about the report to better understand what the data does, and does not, show.
ADVERSE EVENTS
The document itself is an accumulation of post-authorization adverse event reports from Dec. 1, 2020, through to February 2021, taken from the U.S. and other countries, of which there were 42,086 cases in total.
An adverse event is defined as “any untoward medical occurrence that follows immunization,” including an unfavourable or unintended sign such as a skin rash, an abnormal lab finding, symptom or disease.
Dr. Dale Kalina, an infectious disease doctor at Joseph Brant Hospital in Burlington, Ont., told CTVNews.ca in a Zoom interview on Tuesday that Pfizer is required to report any adverse events.
However, just because someone reports an adverse event doesn’t mean it was caused by the vaccine itself.
As the document states, adverse event reports do not necessarily mean they were caused by the drug in question, but could be due to an underlying disease or other factor.
During the Pfizer vaccine trial for those between five and 11-years-old, Kalina says one participant swallowed a penny, which was reported as an adverse event.
“And I think we can all agree that swallowing a penny isn’t related to the vaccine itself,” he said.
“But of course, it highlights the fact that it needs to be reported and that’s what we’re seeing, and that’s the type of data that we’re getting.”
During Modern’s vaccine trials, a 72-year-old participant with arrhythmia, who died after being struck by lightning 28 days post-vaccination, was reported as experiencing a severe adverse event.
Dr. Martha Fulford, an associate professor of medicine at McMaster University, says it’s also unclear in the list whether the adverse events were actually linked to the vaccine or if it was by coincidence.
“I look at this document and I think I sort of come away thinking it’s a little uninterpretable to me,” she told CTVNews.ca in a phone interview on Wednesday.
One of the events listed is hantavirus pulmonary infection, which can occur after coming into contact with rodent urine, droppings or saliva.
“Product availability issue” also is another adverse event on the list.
“Some of that stuff strikes me as highly improbable as doing anything with the vaccine,” Fulford said.
Reporting of adverse events, generally, is underreported, Fulford says, which is something the Pfizer document notes, as well.
But she says it’s unclear how many actual cases of each adverse event were reported or if they appeared at higher rates than what you would see by random chance in the general population.
“The key is whether or not there’s a link and so people reporting something that’s happened, we would need to look at what the overall reported rates would be across a population in a normal period of time,” Fulford said.
THE DENOMINATOR
Both Kalina and Fulford pointed to the lack of a denominator in the document, or in this case how many people received the vaccine at that point in time.
Near the end of February 2021, the United States was vaccinating as many as 1.7 million Americans on average per day, with 63 million Modern and Pfizer vaccines administered.
Looking at the more common adverse events in the Pfizer document, seen in two per cent of cases or more, all are what one would expect after getting a vaccine and when the immune system is excited, namely sore arm, mild fatigue and headache, Kalina says.
The “heaps” of data produced since then around the world have underscored that, he says.
“But to label it as adverse, I think, is a bit of a misnomer because it is actually exactly what you would expect,” he said.
“You’re expecting that reaction and although it’s adverse, it’s not pleasant, it is what you would expect from the medication itself.”
Kalina says any suggestion of a cover-up by Pfizer is being made for “nefarious purposes.”
“It’s a pharmaceutical company, they’re here to make money and I recognize that, there’s no doubt in my mind about that, but the product works,” he said.
While the initial optimism around transmission, for example, has certainly waned as more vaccinated individuals became infected with the Omicron variant, that doesn’t take away from the power of the vaccine to prevent serious disease, hospitalization and death, Fulford says.
“I think most of us, myself included, feel very strongly that for vulnerable people who are at risk from COVID, the vaccines have fundamentally changed what we were dealing with,” she said.
“We saw a huge difference in hospital admissions and severe disease mortality in people who had been vaccinated, this is unquestioned. The risk-benefit conversation obviously changes very much depending on the baseline risk of the person receiving the vaccine, it’s just not an absolute answer.”
WHAT DO WE KNOW NOW?
The Public Health Agency of Canada says that as of Feb. 25, 2022, a total of 40,011 adverse events following immunization have been reported, out of nearly 80.8 million doses administered, for a rate of 0.05 per cent. Most of the adverse effects are classified as non-serious.
At the time the Pfizer report was made, many of those who got the vaccine initially were generally older and potentially vulnerable to COVID-19 infection.
Since then, vaccines have been administered to more, and younger, age groups, providing further evidence to back certain adverse events.
As Fulford says, what needs to be monitored with any medication or vaccine is whether certain signals present at a higher rate than what you would normally see.
This proved to be the case with blood clots and the AstraZeneca vaccine.
Although blood clots can emerge from sitting too long due to travel and certain birth control, their presence after receiving AstraZeneca, while rare, made it distinct, Fulford says.
A similar situation has played out with myocarditis and pericarditis, or inflammation of the heart muscle and lining around the heart respectively.
While also considered rare, people have reported cases after receiving a COVID-19 mRNA vaccine, with higher rates observed following a second dose, among young and adolescent males, and with the Moderna vaccine, the latter possibly due to it being a higher dose than Pfizer.
A report on adverse events from Public Health Ontario shows that rates of myocarditis and pericarditis in males 12-17 and 18-24 after receiving a second dose was 157.9 and 199.4 respectively per million doses, which is roughly two to 13 times higher compared to other age groups.
One recent study also points to the need for individual strategies for vaccinating adolescent boys, due to the elevated risks of myocarditis and pericarditis, and depending on their health and history of COVID-19 infection.
The National Advisory Committee on Immunization recommended in December 2021 that Pfizer be the preferred COVID-19 vaccine over Moderna for those 12 to 29-years-old.
Some studies also have looked into the potential effects of COVID-19 vaccines on women’s menstrual cycles.
Ultimately, Fulford says conversations around the risks and benefits of getting the vaccine will vary depending on the individual.
“It’s not to say that people should or should not be vaccinated, it’s simply acknowledging that yes, we have seen in some people adverse events, and acknowledging that there’s an adverse event is not an all or nothing, and we’ve sort of made it an all or nothing,” Fulford said.
“One can be in favour of vaccines while acknowledging this is the risk in this age group of this adverse outcome, and have that risk-benefit conversation.”
With files from CTV News